|
Peptic ulcer disease - Wikipedia. Peptic ulcer disease. Synonyms. Peptic ulcer, stomach ulcer, gastric ulcer, duodenal ulcer. Deep gastric ulcer. Specialty. Gastroenterology, general surgery. Symptoms. Upper abdominal pain, belching, vomiting, weight loss, poor appetite.   
An “ulcer” is an open sore. The word “peptic” means that the cause of the problem is due to acid. Most of the time when a gastroenterologist is. The most common symptoms of a duodenal ulcer are waking at night with upper abdominal pain or upper abdominal pain that improves with eating. Other symptoms include belching, vomiting, weight loss, or poor appetite. About a third of older people have no symptoms. Bleeding occurs in as many as 1. The diagnosis is typically suspected due to the presenting symptoms with confirmation by either endoscopy or barium swallow. Other conditions that produce similar symptoms include stomach cancer, coronary heart disease, and inflammation of the stomach lining or gallbladder inflammation. 
The medication used to decrease acid is usually either a proton pump inhibitor (PPI) or an H2 blocker with four weeks of treatment initially recommended. Antibiotic resistance is increasing and thus treatment may not always be effective. In case of duodenal ulcers the pain appears about three hours after taking a meal; bloating and abdominal fullness; waterbrash (rush of saliva after an episode of regurgitation to dilute the acid in esophagus - although this is more associated with gastroesophageal reflux disease); nausea, and copious vomiting; loss of appetite and weight loss; hematemesis (vomiting of blood); this can occur due to bleeding directly from a gastric ulcer, or from damage to the esophagus from severe/continuing vomiting. Clinical Guidelines. Authored by a talented group of GI experts, the College is devoted to the development of new ACG guidelines on gastrointestinal and liver diseases. GI Assessment, Diagnosis and Case Studies. Jami Windhorn, RN BSN. SOAR Session #6. Fatty liver and diet Fatty liver, weight loss, and exercise. Medicines associated with peptic ulcer include NSAIDs (non- steroid anti- inflammatory drugs) that inhibit cyclooxygenase, and most glucocorticoids (e. Symptoms of duodenal ulcers would initially be relieved by a meal, as the pyloric sphincter closes to concentrate the stomach contents, therefore acid is not reaching the duodenum. Duodenal ulcer pain would manifest mostly 2–3 hours after the meal, when the stomach begins to release digested food and acid into the duodenum. Also, the symptoms of peptic ulcers may vary with the location of the ulcer and the patient's age. Furthermore, typical ulcers tend to heal and recur and as a result the pain may occur for few days and weeks and then wane or disappear. This pain can be misinterpreted as hunger, indigestion or heartburn. Pain is usually caused by the ulcer but it may be aggravated by the stomach acid when it comes into contact with the ulcerated area. 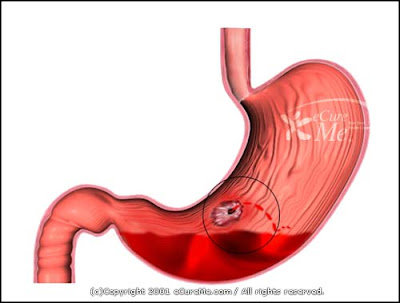
Hi, i am a 42 old female, i experienced gallbladder attacks in oct.2004, was extremely sick, vomiting, lethargy, the ultrasound showed i had alot of gallstones,(30-40. My Dukan Diet Experience (I lost 52 pounds on this diet) by Marshall Brain. I started with the Dukan diet innocently enough. I had read about the diet and wrote an. IFFGD is your resource for reliable digestive health knowledge, support, and assistance about functional gastrointestinal (GI) and motility disorders (FGIMDs). GI for Kids, PLLC is East Tennessee’s premier pediatric gastroenterology group. Located in Knoxville, Tennessee, serve all of East Tennessee and surrounding areas. Peptic ulcer disease (PUD), is a break in the lining of the stomach, first part of the small intestine, or occasionally the lower esophagus. An ulcer in the stomach. HERNIA Minimally Invasive Surgery. A hernia is a hole in the abdominal wall that tissue or organs protrude through. The most common form of hernia is an inguinal. The pain caused by peptic ulcers can be felt anywhere from the navel up to the sternum, it may last from few minutes to several hours and it may be worse when the stomach is empty. Also, sometimes the pain may flare at night and it can commonly be temporarily relieved by eating foods that buffer stomach acid or by taking anti- acid medication. Sudden large bleeding can be life- threatening. Erosion of the gastro- intestinal wall by the ulcer leads to spillage of the stomach or intestinal content into the abdominal cavity. Perforation at the anterior surface of the stomach leads to acute peritonitis, initially chemical and later bacterial peritonitis. The first sign is often sudden intense abdominal pain; an example is Valentino's syndrome, named after the silent- film actor who experienced this pain before his death. Posterior wall perforation leads to bleeding due to the involvement of gastroduodenal artery that lies posterior to the first part of the duodenum. Penetration is a form of perforation in which the hole leads to and the ulcer continues into adjacent organs such as the liver and pancreas. The person often presents with severe vomiting without bile. Cancer is included in the differential diagnosis (elucidated by biopsy), Helicobacter pylori as the etiological factor making it 3 to 6 times more likely to develop stomach cancer from the ulcer. Thus, the bacterium can cause a chronic active gastritis (type B gastritis). Gastrin stimulates the production of gastric acid by parietal cells. NSAIDs block the function of cyclooxygenase 1 (COX- 1), which is essential for the production of these prostaglandins. COX- 2 selective anti- inflammatories (such as celecoxib or the since withdrawn rofecoxib) preferentially inhibit COX- 2, which is less essential in the gastric mucosa, and roughly halve the risk of NSAID- related gastric ulceration. Stress due to serious health problems such as those requiring treatment in an intensive care unit is well described as a cause of peptic ulcers, which are termed stress ulcers. Even when coupled with H. Stomach pain is usually the first signal of a peptic ulcer. In some cases, doctors may treat ulcers without diagnosing them with specific tests and observe whether the symptoms resolve, thus indicating that their primary diagnosis was accurate. More specifically, peptic ulcers erode the muscularis mucosae, at least to the level of the submucosa (contrast with erosions, which do not involve the muscularis mucosae). The tests are typically ordered if the symptoms do not resolve after a few weeks of treatment, or when they first appear in a person who is over age 4. Also, when severe ulcers resist treatment, particularly if a person has several ulcers or the ulcers are in unusual places, a doctor may suspect an underlying condition that causes the stomach to overproduce acid. By direct visual identification, the location and severity of an ulcer can be described. Moreover, if no ulcer is present, EGD can often provide an alternative diagnosis. One of the reasons that blood tests are not reliable for accurate peptic ulcer diagnosis on their own is their inability to differentiate between past exposure to the bacteria and current infection. Additionally, a false negative result is possible with a blood test if the patient has recently been taking certain drugs, such as antibiotics or proton- pump inhibitors. Most labs are not set up to perform H. It is still somewhat controversial whether a positive antibody without EGD is enough to warrant eradication therapy; Stool antigen test; Histological examination and staining of an EGD biopsy. The breath test uses radioactive carbon to detect H. After an hour, the patient will be asked to blow into a bag that is sealed. If the patient is infected with H. This test provides the advantage of being able to monitor the response to treatment used to kill the bacteria. The possibility of other causes of ulcers, notably malignancy (gastric cancer) needs to be kept in mind. This is especially true in ulcers of the greater (large) curvature of the stomach; most are also a consequence of chronic H. This leads to . If the patient stands erect, as when having a chest X- ray, the gas will float to a position underneath the diaphragm. Therefore, gas in the peritoneal cavity, shown on an erect chest X- ray or supine lateral abdominal X- ray, is an omen of perforated peptic ulcer disease. Classification. Esophagus. Muscle. By location. Not associated with acid hypersecretion. Type II: Ulcer in the body in combination with duodenal ulcers. Associated with acid oversecretion. Type III: In the pyloric channel within 3 cm of pylorus. Associated with acid oversecretion. Type IV: Proximal gastroesophageal ulcer. Type V: Can occur throughout the stomach. Associated with the chronic use of NSAIDs (such as ibuprofen). Macroscopic appearance. The ulcer is a round to oval parietal defect (. These borders are not elevated or irregular in the acute form of peptic ulcer, regular but with elevated borders and inflammatory surrounding in the chronic form. In the ulcerative form of gastric cancer the borders are irregular. Surrounding mucosa may present radial folds, as a consequence of the parietal scarring. Microscopic appearance. Ulcer margins are perpendicular and present chronic gastritis. During the active phase, the base of the ulcer shows 4 zones: fibrinoid necrosis, inflammatory exudate, granulation tissue and fibrous tissue. The fibrous base of the ulcer may contain vessels with thickened wall or with thrombosis. In complicated, treatment- resistant cases, 3 antibiotics (e. An effective first- line therapy for uncomplicated cases would be amoxicillin + metronidazole + pantoprazole (a PPI). Most bleeding ulcers require endoscopy urgently to stop bleeding with cautery, injection, or clipping. Epidemiology. Prevalence is higher in third world countries where it is estimated at about 7. Transmission is by food, contaminated groundwater, and through human saliva (such as from kissing or sharing food utensils). The drop in incidence for duodenal ulcers is considered to be a cohort- phenomenon independent of the progress in the treatment of the disease. The cohort- phenomenon is probably explained by improved standards of living which has lowered the incidence of H. Marshall as a causative factor for ulcers. His symptoms disappeared after two weeks, but he took antibiotics to kill the remaining bacteria at the urging of his wife, since halitosis is one of the symptoms of infection. This campaign reinforced the news that ulcers are a curable infection and that health can be greatly improved and money saved by disseminating information about H. Marshall and his long- time collaborator Dr. References. Primary care. PMID 2. 18. 72. 08. Digestive diseases (Basel, Switzerland). PMID 2. 20. 95. 01. Critical Care Medicine. Suppl): S3. 62–4. PMID 1. 20. 72. 66. Gastrointestinal endoscopy clinics of North America. PMID 2. 19. 44. 41. PMC 5. 05. 55. 77 . PMID 2. 77. 33. 28. PMC 5. 38. 89. 03 . PMID 2. 77. 33. 28. National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved 2. 8 February 2. Devaji (2. 01. 4). Clinical Manual of Surgery. Elsevier Health Sciences. ISBN 9. 78. 81. 31. National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved 2. 8 February 2. PMID 1. 88. 37. 77. PMC 4. 34. 06. 04 . PMID 2. 55. 30. 44. Nobel Media AB. Retrieved 3 June 2. SRB's Manual of Surgery. ISBN9. 78. 93. 50. Home Health Handbook for Patients & Caregivers. Merck Manuals. October 2. Atlas: Esophagus. Endoscopic images Copyright . All rights reserved. Logo is Registered Trademark . It does not purport to offer medical advice for any specific medical condition or individual patient. We regret that we cannot provide individualized medical advice online, either via this web site or via email. Please refer to our . See complete Terms & Conditions for use of this website.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
